Facing great demand, Nevada struggles to deliver enough autism treatment
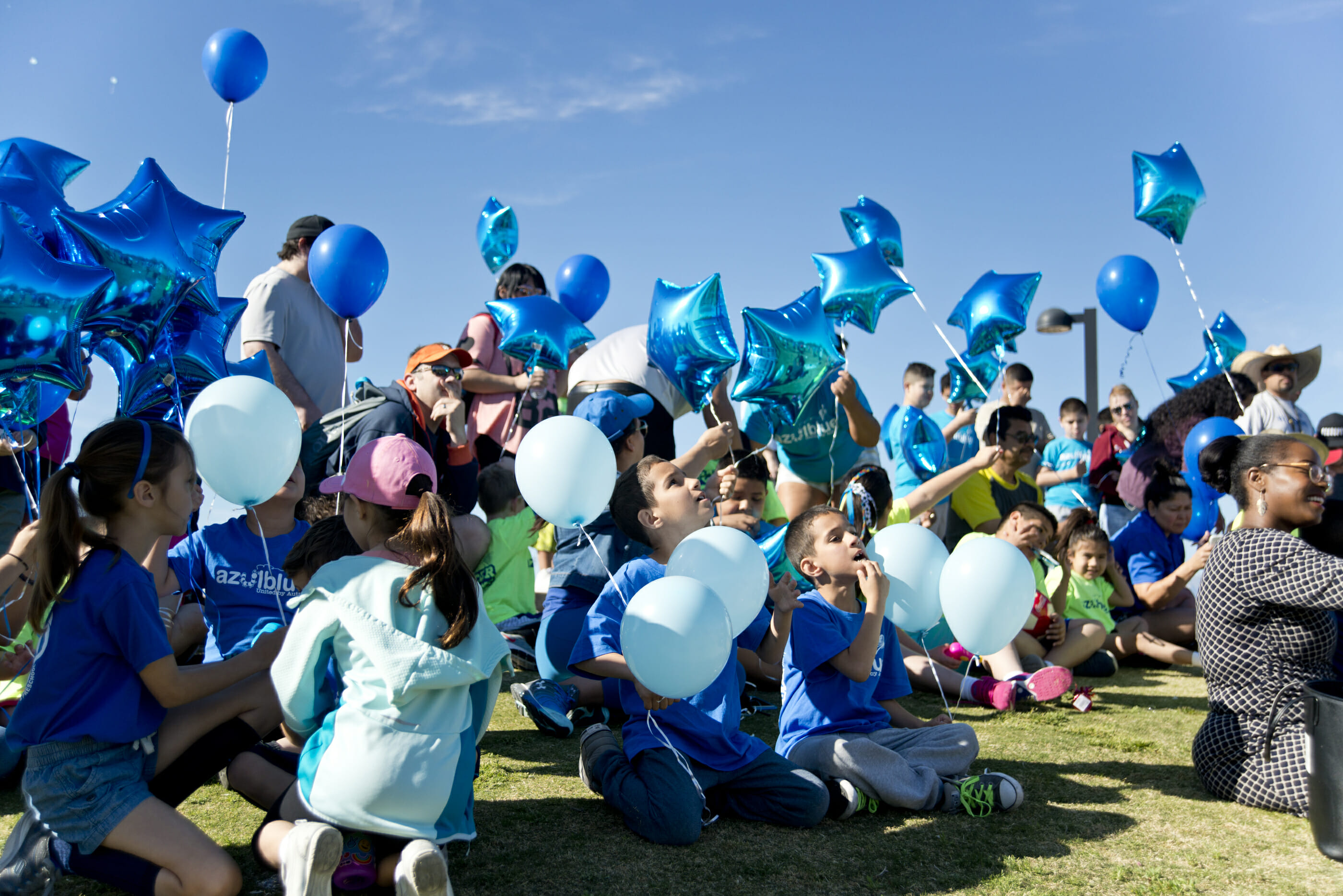
It wasn't long ago when Lynda Tache thought she'd have to lock her son away in an institution.
Diagnosed with autism at age 6, Grant's tantrums and meltdowns frightened her. He was almost 6 feet tall by age 11 and as a single mom, she had nobody to turn to to help restrain him in the middle of his fits.
But that all started to change when he enrolled in the Autism Treatment Assistance Program (ATAP), a decade-old program that helps Nevada families pay for the kinds of one-on-one, sometimes 40-hour-a-week therapies that can manage the bad behavior and cultivate life and social skills in children with autism.
"Now it's a totally different person. He has a great quality of life. He's happy," said Tache, one of several parents who came to the Legislature earlier this month to urge lawmakers to support the program. "ATAP saved our lives."
Tache's current concern is helping Grant, now 15, find his first part-time job this summer. She's also running her own Las Vegas-based nonprofit to help others like him reach their maximum potential and defy a trend of sky-high unemployment among adults with disabilities.
But with nearly 7,000 Nevada public school children between the ages of 3 and 21 diagnosed with autism, the state is hard-pressed to promptly deliver services children need to live normal lives. Treatment for a child might cost $36,000 a year or more, and parents are left to fill in gaps that insurance misses.
Lawmakers will weigh in over the next few weeks on the governor's recommended ATAP budget, which will allow for more children in the program but at about $10 million less than the agency's original request, is far from enough to erase a waiting list.
And while in theory, thousands more children can get help because Medicaid recently started covering the primary therapy for youth with autism, Nevada is serving far fewer children than it thought it would by now because of a workforce shortage and disputes over how much to pay therapists.
As children languish on waiting lists, their progress and potential hang in the balance.
"If we treat kids with autism, they have a chance of becoming independent, tax-paying citizens," said Jan Crandy, a former chair of the Nevada Commission on Autism Spectrum Disorders. "If you don't treat them, they will need some level of support for the rest of their lives. So you're talking a huge cost savings by treating them."
What is autism?

Autism, or autism spectrum disorder, is characterized by challenges with social skills, repetitive behaviors and speech issues, as well as unique strengths. The Centers for Disease Control and Prevention (CDC) estimates 1 in 68 children in the United States have autism, including 1 in 42 boys and 1 in 189 girls.
Around one third of people with autism do not speak, and about one third of people with autism have an intellectual disability, according to the national autism advocacy group Autism Speaks. The condition is often accompanied by physical and mental health issues including gastrointestinal disorders, seizures, sleep disturbances, attention deficit and hyperactivity disorder and anxiety.
There are many types of autism, and the term "spectrum" reflects a wide variety of challenges and strengths possessed by people with autism. One type, Asperger syndrome, is often characterized by clumsiness and an inability to pick up on subtle social cues, but also a precocious vocabulary and obsession with particular subjects.
"The saying is when you meet one person with autism, you've met one person with autism," Tache said. "So they have kind of the same medical deficits, but they are all unique so each child has to have an individualized treatment program."
Autism's most obvious signs tend to surface between 2 and 3 years of age and can include hand flapping, walking on tiptoes, head-banging, consistent fussiness or screaming in public places, repetitive behaviors and little eye contact.

Silvia Rodriguez, who spoke to The Nevada Independent at a recent conference for children with autism, says it can be difficult to leave the house with a child who has the disorder. She recalled an instance in the checkout line at the supermarket when her daughter started throwing groceries.
"That was when a man behind me started to ask why I didn't do something to calm her down," Rodriguez said in Spanish, recalling that the customer suggested she spank the girl. "It made me angry and I wanted to slap him because he spoke out without knowing that, if my daughter's acting like this, it's because of autism."
"I ask, 'why us?' Because it's very difficult. People don't understand that these children are sick," Rodriguez said.
Scientists still don't know exactly what causes autism, which was first described in the 1940s but has been studied much more in recent decades.
The National Institutes of Health says research points to genetic mutations as a likely cause, and says those mutations could increase susceptibility to autism or control the severity of symptoms. Environmental factors, perhaps pesticides or drugs taken during pregnancy, could also play a role.
Erik Lovaas, whose father pioneered one of the most popular methods for treating autism and who now runs the major treatment provider Lovaas Center, said he's seen the number of people with autism shoot up over the past few decades. The prevalence was about 1 in 7,000 when he first started, and he now believes it's closer to 1 in 50 or more, with many people undiagnosed.
"There's a genetic predisposition, but there's something happening in our environment," he said.
Diagnosis and treatment
Experts recommend toddlers between 18 and 30 months old are screened with what's called "M-CHAT" or Modified Checklist for Autism in Toddlers — a series of roughly 20 questions about a child's behavioral patterns. Early clues that a child may have autism include that the child doesn't smile back at a parent, doesn't seem to hear or doesn't point at objects.
A team of professionals can make an official diagnosis, which often comes after observations of a child and interviews with their caregivers. Research indicates early treatment is key and can be far more effective at reducing symptoms than, say, interventions that start at age 6 or older.

Parents including Yolanda Covington swear by Applied Behavior Analysis (ABA). It involves a therapist who teaches new behaviors to a child with autism, redirects repetitive or negative behavior and uses positive reinforcement to build progress.
"It has helped tremendously," said Covington, whose 13-year-old son, Jamari Brown, has Asperger Syndrome. "He's learning to not just be so focused and care about what other people think, what other people's interests are, and not have one-sided conversations."
Children can ease into the therapies as toddlers, starting with 10-15 hours per week and then increasing to 35-40 hours. In the popular Lovaas method, or ABA, an instructor might notice that child takes interest in a toy, then prompt the child to request the toy using appropriate communication.
Therapists also try to interrupt self-stimulatory and repetitive behaviors while still following the child's lead. The goal is to expand communication, cultivate appropriate reactions to sensory input and develop skills such as imitation and requesting.
"You find out what really motivates them, whether it's they get to see a favorite video or write something that motivates the child and then when they have good behavior or they reach a goal ... then you reward them with that," Tache said. "When you punish a typical child and tell them to go stand in the corner or go to your room, they understand what that means. Our children don't. That doesn't register, right? So rewarding them is best."
Benefits big and small
With early intervention, a sizable minority of children diagnosed with autism are able to achieve normal educational and intellectual functioning by 7 years of age.
"It's scientifically supported. Kids can recover from the symptoms, lose the label of autism," Lovaas said.
These children can be mainstreamed into regular classrooms and can be indistinguishable from their peers in social and emotional functioning. Others with more severe cases will never reach the level of their typically developing peers, but therapy can improve their quality of life.

The range of the disorder is obvious among Korri Ward's 23-year-old twin sons who are both diagnosed with autism. Derrick has graduated with a bachelor's degree and is currently working on his master's degree at the University of Nevada, Reno with dreams of becoming a teacher, while Douglas, who also has cerebral palsy, is nonverbal and uses a wheelchair.
He qualifies for a "home and community based waiver," which provides state-funded staff to work with him to ensure he can live at home in spite of his disabilities.
When he was younger, a more highly trained team of staffers encouraged him to interact with people, place his own orders at restaurants and communicate his wants and needs.
"They can program his iPad, so that he can say different things depending on the environment. They make him use his iPad. They have him write schedules. They're respectful of him … and they respond to inappropriate behaviors in a way to help extinguish those inappropriate behaviors," said Ward, who founded the Elko-based Northern Nevada Autism Network. "That helps him feel like he belongs, and that he's important too."
But in contrast to the services offered to people under the age of 22, pay rates are lower for adults with disabilities and attract workers with less training, Ward said. They're less equipped to snuff out bad behavior or ensure Douglas is communicating to his fullest potential.
Ward believes the state needs to raise the rates and the training for staff helping people such as her son, whose most formative years happened before ABA therapies were as common as they are today and perhaps aren't as advanced as they could have been with early intervention.
"The incentive to provide services to adults is less," she said. But "it's just as important for my son to have the behavioral supports ... as it is for somebody that uses a wheelchair to have a cutaway curve."
Medicaid is promising, but rollout is slow in Nevada

For years, insurers resisted covering expensive ABA therapies, declaring them "experimental" treatments. In Nevada, lawmakers scored a victory in 2009 when they passed a bill backed by Democratic Assemblyman James Ohrenschall requiring private insurers to cover up to $36,000 a year in autism therapies, and Republican Gov. Jim Gibbons signed it.
Another victory came when Medicaid, pummelled by lawsuits from families who wanted ABA therapy included in their plans, decided in 2014 that states could cover the time-intensive treatments needed to bring children up to speed with their peers.
Nevada expected to spend about $42 million of its Medicaid budget for autism treatments in the current biennium once the coverage took effect Jan. 1, 2016. The funding was a major component of Gov. Brian Sandoval's plan, announced in his 2015 State of the State address, to get 1,879 kids in treatment.
But with a nationwide workforce shortage and the complex process of providers signing up to serve Medicaid clients, it's been a slow slog to move the money out the door. Through the end of March, there have been just more than $1.2 million in claims from that account (although there is a 180-day lag between when services are rendered and money is drawn from the account). Only 92 children were billing Medicaid for ABA services in the last quarter of 2016 — a fraction of the number hoped.
State officials dispute that anything went wrong, saying they had little information with which to make their projections.
"Originally when we built ABA, it was new across the nation, so no state really had any historical data on what the population would look like," said Shannon Sprout, deputy administrator for the Nevada Division of Health Care Financing and Policy, which deals with Medicaid.
The department came up with a rough caseload projection by checking with the Department of Education on how many children were considered by schools to have autism, and then estimating the percentage that would be eligible for Medicaid. There's room for error in determining the number of children with autism because an "educational diagnosis" used for school count purposes is something less rigorous and formal than a "medical diagnosis."
State officials also say they expected there to be a "ramp-up period." Louisiana and Washington — the first two states to include ABA services in their Medicaid plans — took about 18 months to arrive at full capacity, and Nevada only really started on-boarding its providers last March.
"It was a starting point for us," Sprout said of the 1,879 figure. "We knew coming out that it would be a workforce development issue."
Medicaid money that was designated for ABA services but isn't being used there this biennium is absorbed into treating other, non-autism conditions.. Some wish the money — at least the state matching funds in the ABA budget — could be reapplied to the more nimble, state-run ATAP program, where it could still be used to treat autism as intended.
That's not possible though, as state officials say funds can't be transferred from the Medicaid account to the ATAP program in a totally different state department.
Autism Treatment Assistance Program (ATAP)
ATAP, which started in 2007 as a pilot program and was permanently established by the Legislature in 2011, provides a monthly allotment to pay for therapies based upon a child's individual treatment plan, age, and income.
ATAP generally doesn't pay for all of the recommended hours of treatment, and parents are expected to chip in if they can. In 2014, the actual cost per child per month for ATAP was about $1,500.
The state is budgeting $13 million in the fiscal year that begins this summer and nearly $14 million in the year after that. The general fund contribution is dropping from $8.4 million in the current year to $7.5 million in the second year of the upcoming biennium, with Medicaid funds taking a greater role.
But critics point out that the governor's recommended budget is almost $10 million lower than what the agency had requested. If it included extra money, that could have been used to further pare down a waiting list that averaged about 592 children in the first two months of the year.
State officials say the discrepancy between the request and Sandoval's ultimate budget proposal come because of updates in the caseload projection that happened after the original agency request was made last year.
For example, the agency requested funds to serve 1,164 children in June 2019 — the last month of the biennium. A projection from March 2017 indicates the program would serve 920 children by that point, and the governor's recommended budget makes room for 835.
The caseload projection numbers incorporate the effort to grow the program to accommodate population growth over time. But they start from the current program size, which is often constrained by the budget and a workforce shortage that means providers cannot immediately absorb all the demand for their services.
Caseload projections don't reflect serving every family who seeks services through ATAP; there will still be a waiting list.
There's a sense of urgency among applicants to get children off the list and into treatment, and then keep them in it continuously so their IQs don't drop.
"If there's a disruption in treatment, they actually regress, because it's a developmental disability," Tache said. "That's why we always fight hard every session at the Legislature to at least maintain our funding … These kids have to stay in or else everything we've invested goes away. It doesn't mean anything."
In the first two months of 2017, the program was serving an average of 705 children each month. People who were getting services for the first time have spent an average of 310 days on the waitlist.
"We do have a waitlist in ATAP, but so does every private provider," said Eddie Ableser, director of the Aging and Disability Services Division that oversees ATAP. "It comes back to the fact that the state of Nevada simply doesn't have enough of these professionals to do the work."
The state is trying to move children who are Medicaid-eligible into services paid for by Medicaid, which would free up the resources of ATAP --- mostly general funds — to families who aren't eligible for the federal insurance. But it's not an easy transition because many existing providers can't or won't take Medicaid, which means change-averse children could be pushed off their rolls to a new treatment team.
State officials who oversee ATAP warned providers earlier this month that Medicaid-eligible children who were still using non-Medicaid-enrolled providers would have their funding reduced to a flat $500 a month starting May 1. But they walked that back, vowing this week not to suddenly cut off money for treatment.
"ATAP will continue to fund current Medicaid eligible children who are receiving services through a non-Medicaid provider," they said. "Funding for these children will remain at their current levels until a seamless transition can be made to a Medicaid provider or until a plan decrease is required based on our ATAP plan types."
Anatomy of the workforce shortage
Lawmakers consistently point to a workforce shortage as the root of the problem. Part of it comes because of the recent creation of a nationally recognized credential called the "registered behavior technician" or RBT.
RBTs are paraprofessionals who work directly and usually one-on-one with children with autism. People who have long done such work without a certification have been called "behavior interventionists" in Nevada.
But to get reimbursed by Medicaid, interventionists now must become certified. That means having at least a high school diploma or its equivalent, completing a criminal background check, completing 40 hours of training, passing the RBT Competency Assessment.
In spite of the state's effort to push people toward certification, it's been a slow process to build a robust workforce when nobody had the credential in 2015. Some interventionists are unable to pass the tests, and the ones that do are often snatched up by companies reimbursed by private providers that don't take Medicaid.
While Nevada has an estimated 7,000 children with autism, there are only 145 Medicaid-accepting RBTs as of February.
Compounding the problem is a shortage of Board Certified Behavior Analysts (BCBAs), the professionals who oversee teams of RBTs and design the treatment plans that RBTs implement in the field. There are 53 BCBAs who take Medicaid in Nevada, up from 26 a year earlier.
These professionals must have at least a master's degree in a field such as psychology or education, hundreds of hours of field experience and pass the BCBA exam.
With Medicaid and private insurers now covering ABA services more often, there's an explosion of demand across the country for both of these kinds of workers. A 2015 analysis commissioned by the Behavior Analyst Certification Board found that the number of job postings for behavior analysts more than doubled from 2012 to 2014, increasing from 1,414 postings to 3,083 postings.
Many BCBAs don't take Medicaid because they find Nevada's current reimbursement rates don't make it worth their while.
Cost dispute
Some groups argue that the rate at which the state is reimbursing RBTs is driving a shortage. The state initially set the rate at $29.61, which includes the wage paid to the RBT but also to the employer who must employ a BCBA as a supervisor.
But autism advocates protested, saying the national average reimbursement rate ranges from $40 to $50. The state eventually revised the rate slightly to $31.31 an hour.
Still, the rate is not enough to attract some providers — including the Lovaas Center, which is the largest provider in the state — to start taking Medicaid.
"I think they need to realize they made a mistake with that calculation and go with more national standards," Lovaas said.
A committee that's advising state officials recommended that the RBT rate should be increased to $43.88, as adopted by the military insurance provider TRICARE.
Crandy says that most providers take TRICARE, signaling that it's a viable rate high enough to attract the needed workers to Nevada.
Fixing the pipeline problems

Legislation could also help address a bottleneck in the workforce. Republican Sen. Heidi Gansert is sponsoring SB286, which aims to streamline the licensing process and help RBTs reach for higher certifications.
The bill would create new worker categories, including RBT+, for a person who is studying to become a BCBA. They would get a higher pay rate than a traditional RBT who isn't gaining more experience.
The bill would also create an Applied Behavior Analysis Board closely affiliated with the Aging and Disabilities Services Division. Behavior analysts are currently regulated by the Board of Psychological Examiners, but it's the Aging and Disability Services Division that has oversight of ATAP and other programs directly related to children with autism.
"Our concept is having a board that is responsive to the demand for workforce and streamlining the process for licensing," Gansert said.
The board could help eliminate roadblocks for out-of-state reciprocity, and also come up with strategies to ensure that RBTs who get their national certification with financial help from the state are encouraged to serve the Medicaid population — where the need is greatest.
Nevada has already been investing in helping people become RBTs. The ATAP program has purchased 1,000 licenses to provide online training free of charge to people seeking their required 40 hours of education, and almost 600 have been used so far.
A commission advising the state on autism services wants a few accommodations to help weather the shortage, rather than the hard-line approach of withholding payment to people who don't obtain their RBT credential quickly enough. That includes allowing government payments to behavioral interventionists who are working under the supervision of a BCBA even if they don't yet have the RBT credential — at least until there's a sufficient supply of RBTs.
Reaching underserved communities

Almost 50 percent of Nevada children receiving ABA services through Medicaid are Hispanic, but resources can be hard to come by especially for parents who aren't fluent in English.
Olivia Espinoza has a child with autism and remembers how much time it took to find resources about the condition in Spanish. When she asked another local group if they would start offering information in her native language, they turned her down.
"I asked them if they would help with translators, but they said no because it was expensive," Espinoza said. "I saw that it was time to do something without limits."
In 2011, she founded AzulBlue, which got its official nonprofit status in 2014. Earlier this month, the group put on its fourth annual conference, which offers free workshops on autism — with live translation in Spanish -- featuring doctors who donate their time.
The organization also puts on a soccer camp twice a year that gives children with autism a chance to socialize and build their motor skills. It's called the "Max Soccer Camp" in honor of the Martinez family, who lost their son Max in an accident when he was 4 years old.
Max had autism, and his mother Zaida Martinez is has dedicated herself to families who have trouble finding resources for their children, especially because of their income or language barrier.

Coach Ricardo Mayorga, whose son was diagnosed with autism at age 3, said it's showing results.
"There were some children who couldn't kick the ball, didn't go to the soccer camp, and now they're taking initiative," he said. "A soccer ball is small, but this ball has achieved big results."
Missed opportunities
While some children are able to get the help they need early and see transformative results, others aren't so lucky. Whether it be a language barrier, a misdiagnosis or not enough resources for intensive treatment, some parents are left to wonder what could have been.
That's the case for Rodriguez, who said delays in the health care system and troubles with insurance have stymied progress for her 5-year-old.
"If I had known, I would have placed my daughter in early intervention. But nobody told me, and I didn't know, and the pediatrician didn't help me much. Now after a year a friend recommended another pediatrician who diagnosed her," she said.
Even though she has insurance through Amerigroup, which contracts with Medicaid, there's only coverage for a limited number of therapies and exams, which makes treatment financially difficult. On top of that, there's a language barrier.
"This is also difficult because sometimes they mistreat you and say 'they don't speak English' and ask you to come back with someone who does," Rodriguez said. "I didn't know where to go and nobody guided me."
A man who does work around her house and has a child with autism pointed her to AzulBlue, a support group for families with autistic children. Since then, she's signed her daughter up for speech therapy, occupational therapy and equine therapy.
It's also helped her find more resources for her 2 ½-year-old son, who is receiving speech therapy and is waiting for a diagnosis.
Kimberly Palma-Ortega said it took years before her 17-year-old daughter was finally diagnosed with autism. She thinks her classes should have been more focused on basic life skills that could have helped her be more independent, rather than more academic subjects.
"Right now if you were able to give her services, she is so far delayed," it wouldn't help much, she said.
The focus now is on transitional services that could help her live on her own, perhaps get an internship and live safely. Palma-Ortega is devoting herself to ensuring others don't miss the boat.
"That would be my biggest thing is that what we missed, that we would not allow it to happen to someone else," she said.
For Ward, it's about ensuring families of children in rural Nevada have access to quality care. The shortage of professionals who work with children with autism is even more acute outside Reno and Las Vegas, where delayed diagnoses and waitlists upon waitlists mean children aren't getting treatment until they're 7 or 8 years old.
"We do have families that leave Elko," she said. "You're taking the child with disabilities and his siblings away from a natural support group – the aunts, the uncles, the friends that are in their community – just to access services. And, that's a heartbreak and it shouldn't be requiring people to do that because autism affects 1 in 50 people."
The future
A few years removed from the days when she thought she'd have to send her son Grant away to an institution, Tache is now set on getting him — and others like him — into the workforce.
"It went from us being captive to our home and me being scared to him being happy and living a quality life," Tache said. "If he didn't have (treatment) he probably would have to be institutionalized or he would be with me the rest of his life and he'd have to have services that would cost millions of dollars."
The Grant a Gift Foundation, which Tache launched in 2009 and named after her son, runs training programs to build the social skills that youth with autism will need to succeed in a job. They're up against long odds — 85 percent of adults with a disability are unemployed, and much of the problem is that business owners shy away from the challenge of hiring someone with special needs.
It takes people such as the foundation's chairman, who owns several Subway restaurants and has been supportive of moving young people with autism into jobs there. Participants start with an internship where they can work a few hours at a time and get used to the environment.
The hours build from there. Sometimes, businesses might put a tasteful sign at the cash register asking customers to be patient with employees who might need a little extra time to prepare sandwiches or who might not be smiling all the time.
"I think people naturally are afraid of what they don't know or understand, so I think a lot of employers feel if they hired people with autism or other disabilities that they have to change their business model or they're not going to be as profitable," Tache said. "We're just saying can you like meet us halfway and can this person come into your system with slight accommodations? And then they see, like wow, this is a benefit to our business because it teaches all the other employees around them acceptance and inclusion."
Feature photo: Parents and their children prepare to release balloons during a soccer camp event held by Azulblue at Charlie Frias Park in Las Vegas on Sunday, April 2, 2017. The organization aims to support parents with children in the autism spectrum. By Daniel Clark.
This story was updated May 9, 2017 to add information about how the state projects the ATAP caseload.
Support Independent Journalism in Nevada
You’ve enjoyed unlimited access to our reporting because we’re committed to providing independent, accessible journalism for all Nevadans.
But sustaining this work — informing communities, holding leaders accountable, and strengthening civic life — depends on readers like you.
Nevada needs strong, independent journalism. Will you join us?
A gift of any amount helps keep our reporting free and accessible to everyone across our state.
Choose an amount or learn more about membership

