For Nevada music therapist, rhythm and melody are tools of healing

Editor's note: This article is part of "Nevadans at Work," a video series by The Nevada Independent. Watch more here.
Elizabeth Lenz has been working at the pediatric ICU of Renown Regional Medical Center in Reno since she started working for Note-Able Music Therapy Services three years ago.
For two hours, three days a week, she brings her Radio Flyer wagon full of musical instruments into patients' rooms and offers them a chance to bang a drum or sing a song together.
It might look trivial, but the practice of music therapy has documented clinical benefits. Lenz says doctors have come in the room while she is with a patient and told her they can come back because what she is doing is more important.
"It's so lovely to be part of the team," she says, "and have people actually use you for what you are there for."
The idea that music has healing properties is far from new, but the modern practice of music therapy traces its origins to veterans hospitals after the first and second world wars. Doctors at these hospitals noticed that patients fared much better after being exposed to music. In response to rising demand for trained music therapists, Michigan State University created the first formal degree program in 1944.
During its 2011 session, the Legislature declared that the practice of music therapy is a "learned allied profession" affecting the safety, health and welfare of the public. However, no Nevada college offers a degree in music therapy.
Nevada has a well-documented history of failing to provide adequate mental health services to meet demand. A UNLV study published in February shows Nevada continues to rank last in the nation in overall mental health rankings, despite an increase in funding through federal coronavirus aid packages last year.
A spokesperson for Note-Able Music Therapy Services says their schedule is full and the waitlist for new patients is nearly 55 people long. While some progress is being made, they are having trouble hiring locally because trained music therapists want to live where they know insurance will cover the treatment. Unlike in some states, Nevada Medicaid doesn't cover music therapy.

The American Association of Music Therapists defines music therapy as "clinical and evidence-based music interventions," but misconceptions remain.
"People call us the music ladies," says Lenz. "They think we're just there to sing for people."
While singing to patients is sometimes part of the job, Lenz emphasizes that music therapists are not entertainers. Music is a tool to accomplish specific goals for the patient. The steady rhythm of a song can help people feel safe, and singing encourages deep breathing, which reduces stress.
The first large-scale review of research papers on the neurochemistry of music in 2013 found listening to music to be "more effective than prescription drugs in reducing anxiety prior to surgery." The study also found music improved immune system function and reduced stress levels in patients.
In 2019, the National Institutes of Health, in partnership with the John F. Kennedy Center for the Performing Arts, announced $20 million in grants over five years to support research on the effect of music therapy on neurological disorders.
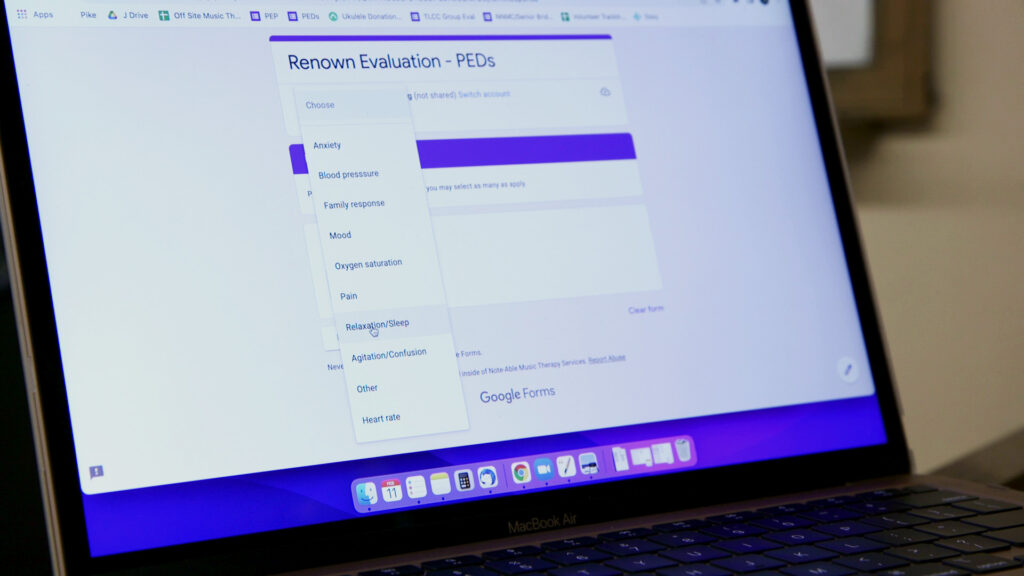
At the end of every day, Lenz catalogs her work in a database — everything from patient blood pressure to emotional state — so Note-Able can track each patient's progress.
During the pandemic, Lenz started working with a woman who suffered a stroke that impaired her speaking, making it hard to communicate with her daughters over Zoom. Lenz still meets with her and uses music to help rebuild the neural pathways damaged by the stroke.
"It doesn't always come out picture perfect," says Lenz. "She still struggles a lot with her speech. But within the session, she was able to tell her daughters that she loves them, and that's something that we practice singing."
Support Independent Journalism in Nevada
You’ve enjoyed unlimited access to our reporting because we’re committed to providing independent, accessible journalism for all Nevadans.
But sustaining this work — informing communities, holding leaders accountable, and strengthening civic life — depends on readers like you.
Nevada needs strong, independent journalism. Will you join us?
A gift of any amount helps keep our reporting free and accessible to everyone across our state.
Choose an amount or learn more about membership
