With opioid-related overdoses on the rise, health care providers try preparing everyday Nevadans to respond to a crisis

Lab coat and webcam on, Atrio Ricarte pushes through his PowerPoint presentation over Webex.
Although the setup on the web conferencing app is reminiscent of a now all-too-familiar online class or working-from-home videoconference, the content the Las Vegas based registered nurse is sharing may just save a life.
From January to May 2020, Nevada saw 23 percent more opioid-related overdose deaths than during the same period in 2019, and similar trends are being seen across the country, prompting the Desert Hope Treatment Center in Las Vegas to host a virtual training on the proper administration of Narcan, a drug intended to treat opioid overdoses. The hour-long training, held on Aug. 26, was intended to help those with or without professional medical training learn more about the drug and be more confident administering it in an emergency situation.
"Narcan is such a simple medication to apply, and it is such a lifesaving variable that we want people to be confident and comfortable with and to know how to use," Derek Price, the chief executive officer of Desert Hope, said.
"Most accidental overdoses occur in a home setting," said Ricarte, who works at Desert Hope. "Most physicians … are very giving as long as there's a certain diagnosis for pain and chronic pain … And having Narcan at home for patients taking these medications is very necessary."
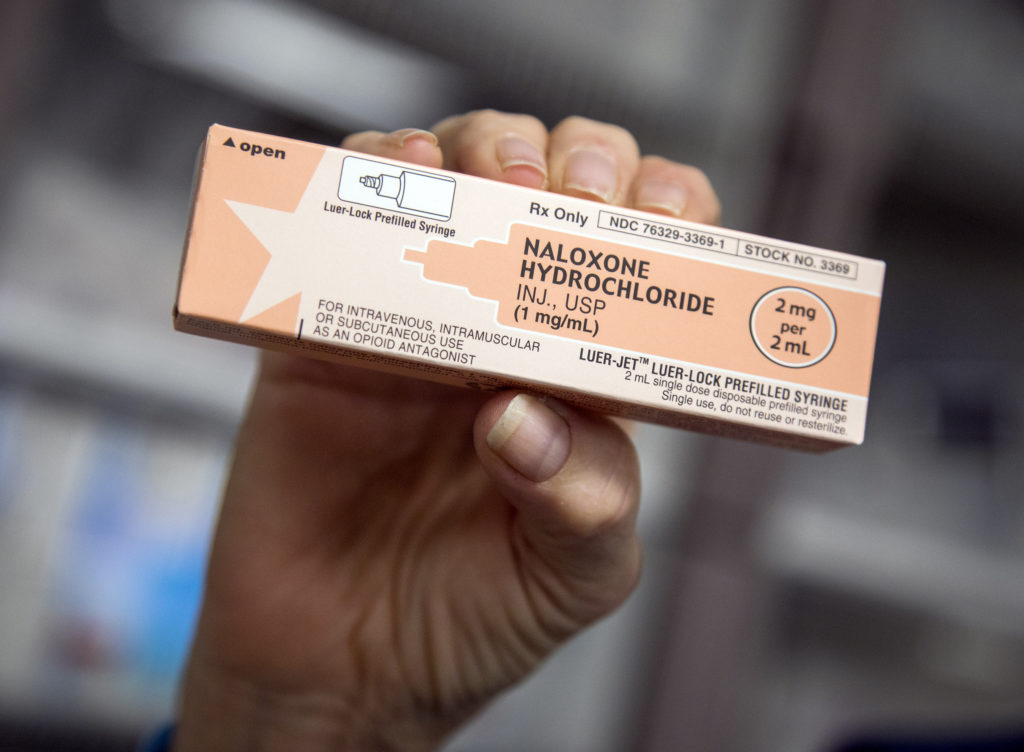
Narcan is one of the brand names for the generic drug naloxone. Naloxone is available in multiple forms but is most commonly distributed as either an injection or a nasal spray.
"It is an opioid antagonist," said Kathryn Barker, senior epidemiologist with the Southern Nevada Health District. "It will actually block the effects that opioids are having in the brain or in the body, so it can reverse an opioid overdose."
The training hosted by Desert Hope covered administration of the Narcan nasal spray specifically, and it was one of several hosted by American Addiction Center, the national company that operates the facility, across the country.
"Our goal is always to educate the community around us on what services we provide, what tools are available, and how best to be ready if any of us is called to action to, you know, save a life," said Michael Burrola, Desert Hope's chief operating officer.
Opioid-related overdose deaths peaked in Nevada in 2011 and have been on the decline since then, but around the U.S., rates have been rising throughout the COVID-19 pandemic. The American Medical Association released a report in mid-August citing news reports from 40 states and Washington, D.C. showing a rise in overdoses and illicit substance abuse since March.
According to data from the Nevada Overdose Data to Action Program, there have been 197 opioid-involved drug overdose deaths in 2020 as of May 31, a 23 percent increase over the 160 counted in the first five months of 2019. April and May had the highest rates of overdose-related emergency room visits, with a 25 percent increase over the three months prior. However, rates have declined since May.
Elyse Monroy, manager of the Nevada Overdose to Action program, said in an email to The Nevada Independent on Thursday that it is "difficult to say for certain" based on these statistics whether the COVID-19 pandemic had a direct effect on rates of hospitalization and death. However, she did say anecdotally that limited access to treatment centers and changes in availability of the illicit drug supply seem to have affected the rates.
While the statistics may not say for sure, health care providers throughout the country believe that increased stress and isolation, both mentally and physically, as a result of the pandemic have influenced rates of drug abuse and overdose, and Price is among them.
"We have a global pandemic that we've never faced before. With that comes fear, anxiety, and depression," Price said. "When you put people under more stress, anxiety, and fear, the people that have a substance abuse issue … are only going to find an increase in the desire for utilization."
One report cited by the medical association came from the Southern Nevada Health District, which announced that there were 63 deaths involving fentanyl from the beginning of the year through the end of May, compared to 28 deaths during that same period in 2019 – a 125 percent increase.
Often used as a pain reliever, fentanyl is a synthetic opioid similar to morphine but far more potent. According to Barker, the added danger fentanyl poses in Clark County and around the country is that other drugs will often be laced with the substance.
"Fentanyl is a potent opioid. In its prescription form it's used to treat cancer pain," Barker said. "But when it's illicitly manufactured, it's often mixed into other drugs."
While deaths from prescription opioids had been decreasing both in the state and nationally based on preliminary numbers from 2019, deaths involving non-prescribed synthetic opioids are on the rise. From January to June 2020, there were 197 overdose deaths in the state and 102 of those involved fentanyl.
"It is not unfair to say that Fentanyl alone has turned prevention and intervention efforts on their head," Monroy said "Law enforcement in both the North and the South have reported to our public health partners that 'fentanyl is everywhere.'"
According to Monroy, the state is pivoting its focus from heroin and opioids towards stimulants such as methamphetamine and cocaine which have been laced with fentanyl.
"We are trying to spread the word that there is fentanyl in our community, and it's potent, and it can lead to fatal overdoses," Barker said.
Because of the risk of unknowingly overdosing on the drug, the health district advises that anyone who uses illicit substances or knows someone who does, even if they are not seeking out opioids themselves, keep naloxone on hand for use. Health professionals, including Ricarte, also encourage anyone who has been prescribed opioids, or has a loved one who has, should also have naloxone available. Nevadans can purchase Narcan and other forms of naloxone through a pharmacist without a prescription or get it free at a distribution site.
Narcan and other forms of naloxone also typically come with instructions either in written or video form. According to Barker, the risks associated with the drug are low, and anyone administering the drug who is informed about how to use it should be able to do so safely and effectively.
Still, she emphasizes that the drug alone may not be sufficient treatment and patients may immediately enter a withdrawal. For that reason, anyone administering the drug should always call 911 or get the patient to a hospital.
"Narcan isn't a permanent medication that would help through the whole overdose. It's only temporary," Ricarte said in Desert Hope's training. "It might work for about 10-15 minutes, and then it could get even worse if not treated with emergency medical care."
The Nevada Department of Health and Human Services operates a virtual naloxone dispensary where distributors can order the drug, and Nevadans can find a nearby community-based distribution site online. The Southern Nevada Health District points those in Clark County toward harm reduction centers such as Trac-B exchange, which offers counseling and syringe exchange in addition to naloxone distribution.

While Desert Hope's outreach efforts have been limited as a result of the COVID-19 pandemic, the treatment center is hoping to resume its normal events and operations and expand its online offerings.
"Our primary focus is always to target the family and educate them on tools and resources available," Burrola said. "Narcan is obviously the dominant factor… However, there's other resources we cover in terms of support tools."
The Narcan training, in particular, is intended to be an annual event to help individuals understand the purpose of the drug and gain confidence in administering it.
"Getting Narcan and keeping it in the house … it's kind of like having a fire extinguisher," Price said. "You pray you never have to use it, but you're sure that it's there when you need it."
Support Independent Elections Coverage and Journalism in Nevada
You’ve enjoyed unlimited access to our reporting because we’re committed to providing independent, accessible journalism for all Nevadans.
But sustaining this work — informing communities, holding leaders accountable, and strengthening civic life — depends on readers like you.
Nevada needs strong, independent journalism. Will you join us?
A gift of any amount helps keep our reporting free and accessible to everyone across our state and funds our elections coverage.
Choose an amount or learn more about membership
