Nevada's most vulnerable people are at risk when public health emergency ends
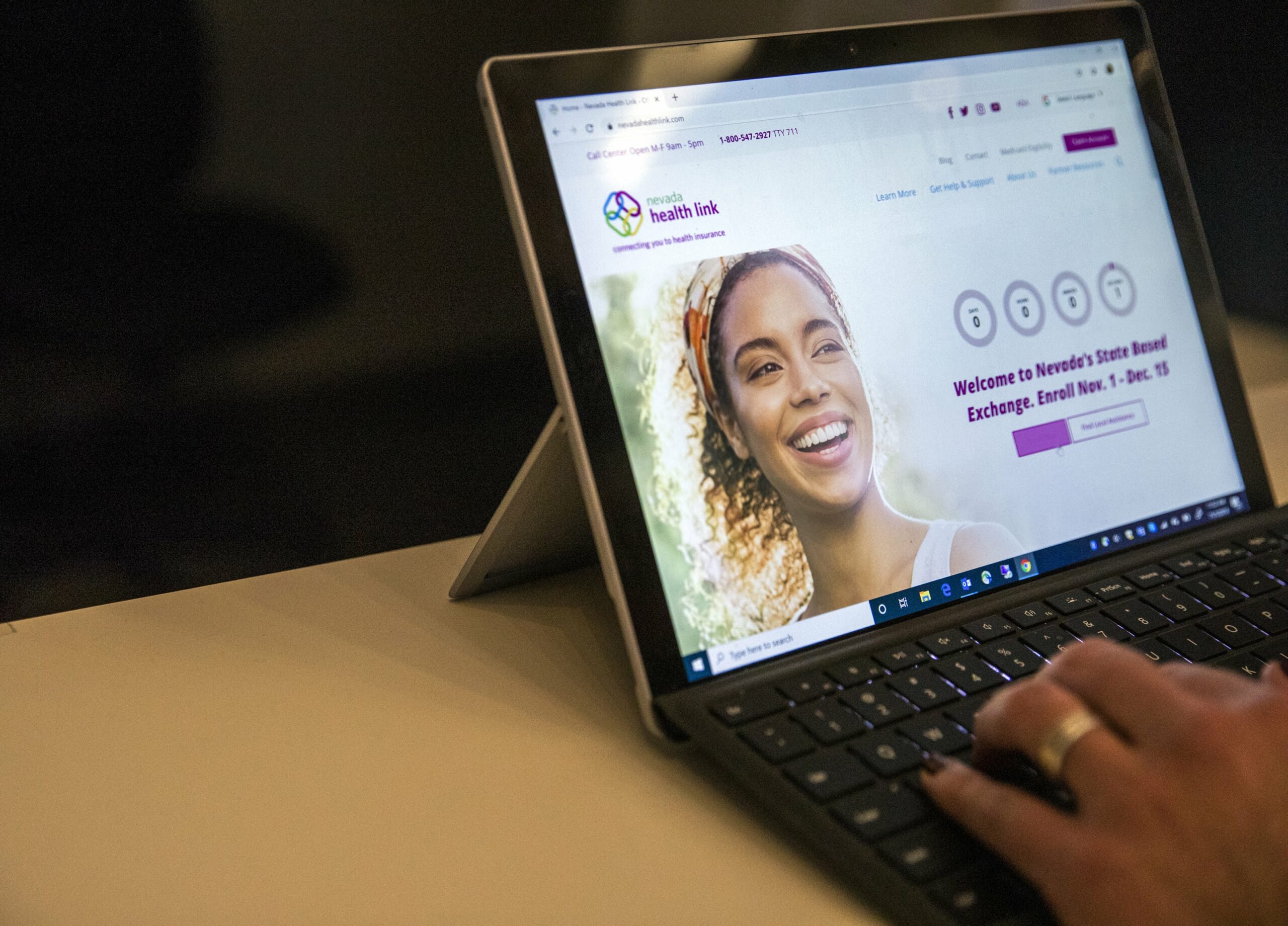
Nevadans have good reason to cheer: COVID cases and hospitalizations are declining in the state, leading Gov. Sisolak to rescind the mask mandate. But with this good news comes a dose of reality – millions of Americans who gained affordable health insurance coverage over the past two years thanks to significant federal relief programs are at risk of losing their coverage. This could lead to dire financial or medical consequences for the nearly 1 million Nevadans enrolled in Medicaid or Nevada Check Up, and risks inundating state health systems.
The federal government declared a public health emergency (PHE) for COVID-19 on January 31, 2020 and has since extended it eight times. Now, the PHE is set to expire some time this year. A key goal of the PHE was to help low-income families and children receive appropriate preventive and primary care during the pandemic without disruptions in coverage. To do that, the PHE required states to keep Medicaid enrollees continuously covered, irrespective of their circumstances.
Nationally, enrollment in Medicaid and the Children's Health Insurance Program (CHIP) grew to a record high of an estimated 83 million individuals as of last December, primarily due to the continuous coverage requirements of the PHE. In Nevada alone, more than 810,000 individuals are enrolled in Medicaid or Nevada Check Up, an uptick from 671,979 before the pandemic. The American Rescue Plan Act, passed by Congress last year, was another step to help keep financially struggling Americans insured. The legislation provided premium subsidies to those who purchased health insurance from public marketplaces, making it more affordable than ever. Millions of families saved $2,400 per year in health insurance premiums.
Both policies provided a safety net these last two years for struggling Americans. When the PHE ends, so too will the continuous coverage for Medicaid enrollees and millions will find themselves without health insurance. When the American Rescue Plan subsidies expire at the end of this year, premiums could double, and many individuals and families may drop their insurance.
A perfect storm is brewing. If marketplaces don't adequately prepare for this influx, millions of Americans could lose health insurance and may forgo necessary preventive care, leaving them more vulnerable to illness and injury while the state's hospitals and doctors will be left without a payment source for treatment. The economic consequences of an uninsured constituency ripples beyond the health care sector, impacting productivity and adding to the nation's deficit.
To address the PHE, Nevada and states across the country will have to help low-income individuals reapply for Medicaid or get connected to Nevada Health Link to get access to Affordable Care Act subsidized health insurance plans. State and federal health and human services agencies—many of which are already understaffed and using antiquated IT systems—need to work together quickly to prepare for this massive effort.
States like Nevada that have their own exchanges, which I was proud to help create, will be better prepared to transition people to marketplace insurance—but the whole of state health and human service agencies need to leverage existing technology and resources to be prepared and mitigate coverage loss.
Most government agencies have disparate legacy eligibility and enrollment systems that do not share data. This delays the processing and delivery of essential benefits that millions of Americans rely on. State agencies must have the support and budget needed to upgrade their technology and deploy more efficient processes, so that the upcoming challenges don't overwhelm their ability to provide services.
Nevada and other state-based marketplaces today rely on modern technology that can automate processes, such as pre-populating applications or using other trusted sources of data to make eligibility determinations, which enable consumers to easily enroll in affordable plans and complete the transition from Medicaid to a marketplace plan. In Nevada, for instance, enrollees can opt for automatic renewal and can complete a universal eligibility application for Medicaid and food benefits.
As part of the American Rescue Plan, Congress also added $1 billion to the Technology Modernization Fund to modernize public-facing IT services. States must start utilizing the available funds and begin actively working to automate, streamline, and reduce manual interventions, learning from places like Nevada.
The stakes are high for millions of Americans and the clock is ticking. Without proper planning, the country is looking at the perfect storm of coverage loss undoing years of progress in the blink of an eye.
Heather Korbulic is the senior policy and strategy lead at GetInsured, where she engages local, state, and federal health care policy leaders in developing strategies for technology-driven improvements to the provision of health care and other public benefits. She was previously the executive director of Nevada's health insurance marketplace, the Silver State Health Insurance Exchange.
Support Independent Journalism in Nevada
You’ve enjoyed unlimited access to our reporting because we’re committed to providing independent, accessible journalism for all Nevadans.
But sustaining this work — informing communities, holding leaders accountable, and strengthening civic life — depends on readers like you.
Nevada needs strong, independent journalism. Will you join us?
A gift of any amount helps keep our reporting free and accessible to everyone across our state.
Choose an amount or learn more about membership

