Facing shortened timeline, Nevada's exchange, brokers gear up for Obamacare open enrollment
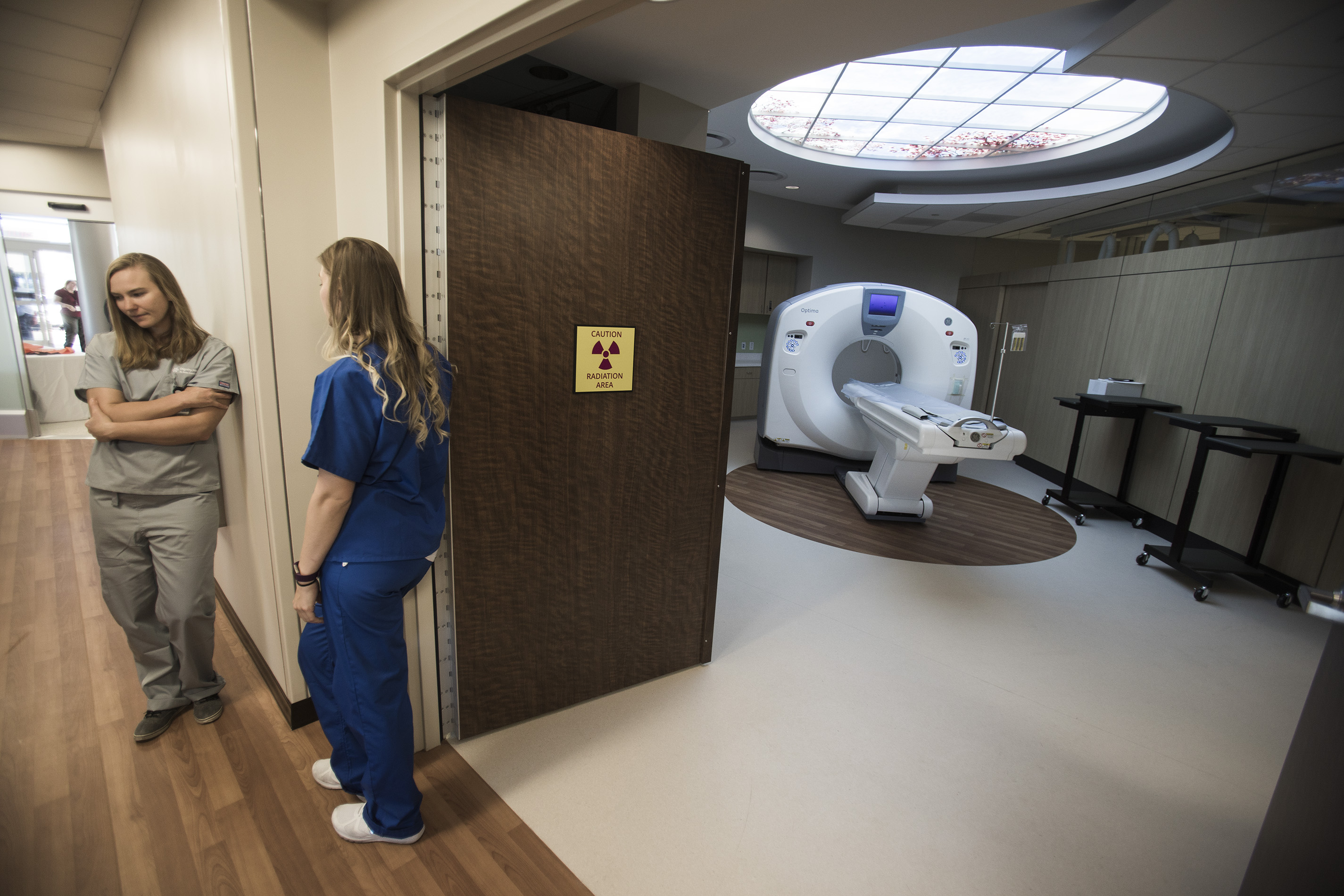
Against a backdrop of months of congressional debate and executive action on Obamacare, Nevada's health insurance exchange, brokers and other advocates are battening down the hatches ahead of the sixth open enrollment period — and what could be the most challenging one yet.
This year, Nevada lost two insurance providers on the Obamacare exchange, saw one company plan to offer coverage before later backing out and briefly faced the threat of roughly 8,000 residents in 14 counties having no on-exchange insurance options at all. Though all counties now have at least one insurer offering plans for the coming year, Nevadans still have fewer choices, less time and more information to sift through headed into open enrollment this year than ever before.
On top of that, open enrollment, which runs from Nov. 1 to Dec. 15, is only half the length this year of what it has been in the past due to a rule change by the Trump Administration, and the federal website used to sign up for insurance plans, healthcare.gov, will shut down for maintenance overnight on the first day of open enrollment and 12 hours most Sundays during the 45-day period. For brokers and other assisters tasked with helping people choose the health plan that's best for them, that means double the demand on any given day.
In Nevada, roughly 122,000 people have individual health plans (including more than 88,000 on the exchange), meaning they are not covered under an employer-sponsored health plan, Medicaid or Medicare. That amounts to more than 2,700 people a day in Nevada who may need assistance signing up for the right health plan on any given day of open enrollment.
To top it off, some brokers and advocates say there's significant concern among members of the general public about what kinds of insurance they'll be able to purchase this year, how much it will cost them and — at the most extreme — whether the Obamacare exchange still exists at all.
"There's a lot of confusion out there, people thinking the program doesn't exist in general anymore. Is it going to be around next year? Are rates going to increase?" said insurance broker Albert Ochoa. "That's why I think it's important for us to be able to bring that information to them and keep them as comfortable as they can possibly be with the process."
Ochoa's brokerage firm was one of three organizations selected by the state's exchange as part of a pilot grant program to increase outreach to consumers and set up storefronts during open enrollment where people can come for help. It's all part of an effort to, in the words of Silver State Health Insurance Exchange Executive Director Heather Korbulic, "cut through the noise."
"We're cutting through the racket and making sure that people understand there are still plans on the exchange and still subsidies available to them," Korbulic said. "What you're hearing from the media and what you're hearing from Washington D.C. is noise. We want you to know you should be insured to protect yourself."
The logistics
Nevadans, depending on where they live in the state, will either have one or two insurance providers available to them on the Obamacare exchange. Residents in all 17 counties can purchase SilverSummit plans, while residents in Clark, Nye and Washoe counties will also be able to purchase coverage through Health Plan of Nevada.
SilverSummit, a subsidiary of Centene, agreed in August to step in and provide coverage to the 14 rural Nevada counties that had been left bare of any on-exchange insurance coverage after Anthem announced in June it was scaling back coverage before eventually pulling out of the state altogether. Across the country, Centene has expanded its presence on insurance exchanges as other companies have scaled back or abandoned individual market coverage altogether by offering low-premium, high-deductible plans. More than 90 percent of its exchange customers are eligible for federal subsidies, including many who rotate in and out of Medicaid, the company's core business.
Even still, residents in Clark, Washoe and Nye counties are down from three options on exchange to two. Rural residents are down from either two to one, or only had one option on the exchange to begin with.
People can also purchase insurance off exchange but can't use any federal subsidies for which they may qualify there, which means they'll be paying the full sticker prices. Still, off-exchange plans may give people whose incomes are too high to qualify for subsidies additional flexibility when it comes to choosing a plan with benefits best for them or may even be worth the cost for someone who is eligible for subsidies.
In Clark County, people can purchase off-exchange plans through Health Plan of Nevada, Hometown Health and Sierra Health and Life. In Washoe, only Health Plan of Nevada and Hometown Health are available off exchange. Some of the rural counties, such as Esmeralda, only have catastrophic plans offered off exchange through Anthem, a high-deductible health plan for people under 30 who qualify for a hardship exemption.
"The people who live in the rurals unfortunately will have one option. They have SilverSummit. That's it," said Heidi Sterner, the immediate past president of the Clark County Association of Health Underwriters. "It gives them literally one option. You hate to say people in Clark County and Washoe County should be thanking their lucky stars that they have more than one option, but that's the case."
To boot, Nevada's health insurance rates have increased for next year to account for the fact that insurance companies will no longer receive payments from the federal government that help health insurance companies offer affordable coverage to low-income Americans. The state Division of Insurance opted to assume the so-called cost-sharing reduction payments would end when it set rates for the coming year, leaving Nevada in less of a lurch than other states when the president announced the payments would end this month.
But people currently receiving federal subsidies shouldn't feel much, if any, impact, exchange officials say. Adjustments to the advanced premium tax credit, a sliding scale tax credit to help individuals and families with moderate income afford health insurance, should account for the loss of the cost-sharing reduction payments. (An individual can make up to $47,080 a year and still qualify for the credit, while a family of four can make up to $97,000.)
The people who aren't subsidized, however, will have to bear the full burden of the rate increase, about a 31.6 percent increase for plans both on and off the exchange. Health Plan of Nevada, the only on-exchange plan to carry over from 2017, increased by 36.8 percent over the last year.
The problem is, as Sterner and other brokers have already seen this year, is that as rates go up for plans that offer less coverage, more and more people are considering taking the tax penalty and foregoing insurance altogether. In 2017, the tax penalty is 2.5 percent of a household's income or $695 per adult and $347.50 per child for a maximum of $2,085, whichever is higher.
And it's not just affecting people who don't receive subsidies. Sterner said she knows people whose ending premium was $50 and that was still too much to afford.
"Honestly it's going to come down to, 'Do I pay my mortgage or for food and fuel in my vehicle so I can get to and from work or am I going to pay health insurance?'" Sterner said. "I think people are going to have to make that tough choice, and it's really going to be hard for them. It's sad."
Finding the right coverage
The health exchange, brokers, in-person assisters and navigator organizations are all giving the same advice to those looking to either enroll or re-enroll in a plan on the exchange: Get help, and don't wait to do it.
"My same message multiple times is don't be confused. Just get connected to a health insurance professional and get enrolled," Korbulic said.
Korublic is encouraging everyone to shop the marketplace (open for window shopping now), particularly those people whose insurance carrier has left the market and are slated to automatically be rolled onto a similar plan with a different provider. A new insurance company means different doctors, a different list of approved medicines and different costs for services.
But comparing the nuances of health insurance plans can be tricky, which is why the exchange recommends that people get connected with an insurance broker, in-person assister or navigator instead of trying to navigate the enrollment website on their own. For instance, someone might be inclined to choose a plan that saves $20 a month in premiums but not realize the prescription medication he or she takes costs $50 a month more on that cheaper plan.
The Community Health Alliance, an in-person assister organization certified by the state to help people sign up for plans on the exchange, has already seen calls come into its call center from people concerned about what ending the cost-sharing reduction payments means for their insurance and has seen more applicants are opting to choose bronze plans — those with the lowest monthly premiums but highest costs for the patient when they need care — than before, says CEO Chuck Duarte. The alliance has three people who will travel throughout Washoe County rotating through churches, social service agencies and a call center to provide assistance to people during the shortened open enrollment period.
"It crowds people out of coverage if they can't get assistance. A lot of brokers aren't doing this type of work anymore," Duarte said. "So that's really the big concern, and what we're trying to do right now is promote the fact that it's a short open enrollment period and that people need to act."
Meanwhile, the state Office for Consumer Health Assistance is responsible for overseeing four navigator organizations, which not only provide information like in-person assister organizations but can actually enroll people in a health insurance plan online. There are three navigator organizations in southern Nevada and one in Elko that serves the rurals, from Battle Mountain to Carlin.
"We're doing a lot of appointments and scheduling appointments ahead of time," said Janise Wiggins, the governor's consumer health advocate. "Not that we won't accept walk in appointments, but we're going to be hustling every single day to get as many people enrolled as possible."
The six ombudsmen who work in the office, five in Las Vegas and one in Elko, are also responsible for helping the people who fall through the cracks, like undocumented immigrants or seniors who don't qualify for Medicare. The ombudsmen also help sort out issues with insurance companies, such when a certain procedure or a drug isn't covered.
"We're a pretty small and boutique office compared to some other Department of Health and Human Service agencies," Wiggins said. "The benefit is we can slow down, I think, a little bit and not always do things in such a rigid systematic way that we can customize the service that people need so we can stop them from being on a hamster wheel going from agency to agency and agency never getting to the root cause of the issue."
At the same time brokers, like Ochoa, will continue focusing on the immediate task at hand — getting people enrolled. Ochoa's firm has hired additional brokers and will be open from 10 a.m. to 8 p.m. at the Boulevard Mall trying to reach as many people as possible and get them enrolled by the Dec. 15 deadline.
"One of my biggest fears is that people will miss the open enrollment," Ochoa said.
An eye on the federal level
While Republicans work to dismantle the Affordable Care Act and Democrats fight to keep it in place, most professionals in the health-care industry agree that the federal health-care law is flawed and in need of fixing, even as open enrollment moves ahead this year.
"We have been advocating for bipartisan efforts to repair the Affordable Care Act for months and months and months," Sterner said of the National Association of Health Underwriters lobbying efforts at the federal level.
One bipartisan deal from Republican Sen. Lamar Alexander from Tennessee and Democratic Sen. Patty Murray from Washington would continue to fund the Affordable Care Act's cost-sharing reductions while allowing states more flexibility.
But President Donald Trump has waffled on whether he would sign the Alexander-Murray deal into law, which now has 12 Democrats and 12 Republicans as co-sponsors. Last week, he said he wouldn't continue the cost-sharing reduction payments before saying a few minutes later that the bipartisan deal is "a very good solution." Hours later, he urged Congress to "find a solution to the Obamacare mess instead of providing bailouts to insurance companies."
Though not a co-sponsor, Democratic Sen. Catherine Cortez Masto tweeted that Alexander-Murray will help stabilize the health-care market and ensure premiums don't rise, calling it a "good step in the right direction."
Republican Sen. Dean Heller's office did not respond to a request for comment about whether he supports the proposal, though fellow Republican Gov. Brian Sandoval has urged Congress to act on the measure in a letter with a bipartisan group of nine other governors.
"We urge Congress to quickly pass legislation to stabilize our private health insurance markets and make quality health insurance more available and affordable. Senators Alexander and Murray have negotiated in good faith and developed a bipartisan agreement that will help achieve these goals," Sandoval and the other governors wrote in the letter. "Their legislation deserves a vote by the House and Senate."
Support Independent Journalism in Nevada
You’ve enjoyed unlimited access to our reporting because we’re committed to providing independent, accessible journalism for all Nevadans.
But sustaining this work — informing communities, holding leaders accountable, and strengthening civic life — depends on readers like you.
Nevada needs strong, independent journalism. Will you join us?
A gift of any amount helps keep our reporting free and accessible to everyone across our state.
Choose an amount or learn more about membership
